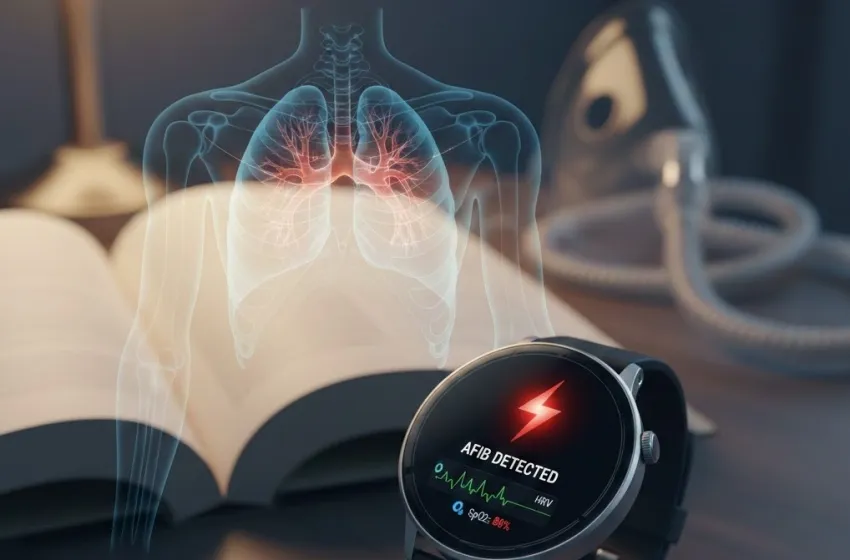
Explore the cardiovascular link between irregular heart rhythm and severe sleep apnea via HRV and SpO2 monitoring.
The rise of wearable tech has revolutionized personal health monitoring. Beyond counting steps and calories, modern smartwatches and fitness trackers are increasingly equipped with sophisticated sensors capable of providing critical insights into our physiological state. One of the most touted features is the ability to monitor Afib detection, or atrial fibrillation—an irregular heart rhythm that is a major risk factor for stroke.
However, the information gleaned from your wrist might be telling a deeper story than just a quirky heart flutter. Emerging research is shedding light on a profound and sometimes surprising cardiovascular link between an irregular heart rhythm and underlying respiratory conditions, particularly sleep apnea screening and chronic lung strain. Could your smartwatch, in its vigilance against Afib, be providing early warning signs of a potential lung issue? The answer, increasingly, seems to be yes.
The Silent Epidemic: Understanding Atrial Fibrillation (Afib)
Atrial fibrillation is the most common sustained cardiac arrhythmia, affecting millions globally. In a healthy heart, the atria (the upper chambers) contract regularly. In Afib, the atria beat chaotically and irregularly, leading to poor blood flow and the potential formation of clots.
While often treated as a primary heart condition, Afib is frequently a symptom, a visible consequence of broader systemic stressors. The electrical and structural remodeling of the heart that leads to Afib is profoundly influenced by chronic stress, inflammation, obesity, and, critically, respiratory stress.
The Connection Between Heart Rhythm and Respiratory Stress
The heart and lungs are intimately linked, physically and physiologically. They operate in a delicate, balanced feedback loop known as the cardiopulmonary system. The health of one directly impacts the function of the other.
The Role of the Autonomic Nervous System
The most crucial intermediary in the Afib-respiratory connection is the autonomic nervous system (ANS), the body’s control center for involuntary functions like breathing and heart rate.
- Vagal Tone and Parasympathetic Stress: Severe respiratory stress, such as that caused by sleep apnea, triggers an overactivation of the parasympathetic nervous system (PNS), often referred to as the "rest and digest" system. During periods of low oxygen (hypoxia) at night, the body attempts to protect itself by dramatically slowing the heart via the vagus nerve. This sudden, excessive increase in vagal tone is a potent trigger for Afib episodes, particularly those that occur at night.
- Sympathetic Nervous System (SNS) Compensation: Conversely, the daytime strain and chronic oxygen deprivation can activate the sympathetic nervous system (SNS), the "fight or flight" response. This constant state of alert releases catecholamines (stress hormones) that increase heart rate and blood pressure, leading to electrical instability in the heart muscle.
Physical and Mechanical Strain on the Heart
The respiratory system can physically strain the heart, especially the left atrium, which is the most common site where Afib originates.
- Pulmonary Hypertension: Chronic lung diseases (like COPD or severe sleep apnea) can cause blood vessels in the lungs to constrict, leading to pulmonary hypertension (high blood pressure in the lungs). This back-pressure forces the right ventricle of the heart to work harder.
- Left Atrial Remodeling: The mechanical strain from this increased pressure and the swings in intrathoracic (chest) pressure during a struggle to breathe (a hallmark of sleep apnea) cause the walls of the atria to stretch and dilate. This stretching, or remodeling, creates the ideal substrate—electrically unstable and structurally compromised tissue—where Afib can easily take hold. This explains why irregular heart rhythm (Afib) often co-occurs with severe sleep apnea and lung strain.
How Irregular Heart Rhythm (Afib) Often Co-Occurs with Severe Sleep Apnea and Lung Strain
The co-occurrence of Afib and sleep apnea is not a statistical anomaly; it is a clinical expectation.
"Studies have consistently shown that patients with obstructive sleep apnea (OSA) have a two- to four-fold increased risk of developing Afib compared to the general population. Furthermore, Afib treatment, including ablation, is significantly less successful in patients whose sleep apnea remains untreated."
The Sleep Apnea-Afib Cycle
- Apneic Events: A person stops breathing or has dramatically shallow breathing for seconds during sleep.
- Oxygen Desaturation: Blood oxygen levels plummet (hypoxia).
- Vagal Surge: The brain registers the emergency and tries to shock the system back to breathing by triggering a strong vagal response, causing a sudden, dramatic drop in heart rate (bradycardia).
- Arousal and Catecholamine Surge: The person gasps awake, leading to a massive sympathetic surge, raising heart rate and blood pressure instantly.
- Pressure Swings: The forced inspiration against a closed airway (the mechanism in OSA) creates extremely negative intrathoracic pressure, essentially "sucking" on the heart, leading to acute strain and further atrial stretching.
This repeated, nightly cycle of hypoxia, pressure swings, vagal activation, and sympathetic overload is the perfect electrical and structural storm for triggering and sustaining Afib.
The Smartwatch as a Respiratory Pre-Screening Tool
This is where your wearable tech becomes an invaluable, passive early warning sign system, acting as an unintended sleep apnea screening device.
The primary feature, Afib detection via photoplethysmography (PPG) sensors (or in some cases, single-lead ECG), is designed to spot the irregular electrical activity of the atria. Crucially, Afib episodes linked to sleep apnea often occur *exclusively* during the night. A smartwatch that repeatedly alerts the user to nocturnal or early morning Afib, especially in an otherwise healthy or mildly symptomatic person, should immediately raise the suspicion of underlying sleep-disordered breathing.
One of the most powerful yet often overlooked metrics provided by advanced wearable tech is heart rate variability (HRV). HRV is the measure of the time difference between successive heartbeats. It is the gold standard for non-invasively assessing the health of the autonomic nervous system.
While not all wearables have it, those equipped with blood oxygen saturation (SpO2) monitoring further strengthen the case. Repeated drops in SpO2 below 90-92% during sleep—often logged as an "abnormal reading" or "respiratory event"—coupled with Afib or low HRV readings, create a powerful combination of early warning signs that warrant a formal sleep study.
- Afib Detection and Nocturnal Arrhythmias
- Heart Rate Variability (HRV) Analysis
- Sleep Apnea's Impact on HRV: Sleep apnea causes a profound and specific disruption to the ANS. During the apneic event, the HRV becomes highly erratic due to the vagal/sympathetic surges. Over time, the chronic stress exhausts the ANS, leading to a persistently low HRV (reduced variability) both during the day and night.
- HRV as a Risk Predictor: A smartwatch showing a consistently low nocturnal and resting HRV—often trending downward over months—can be a strong, non-specific indicator of chronic systemic stress, with respiratory stress being a primary suspect. The smartwatch isn't directly measuring oxygen, but it's measuring the heart's stressed *reaction* to low oxygen.
- Oxygen Saturation (SpO2) Monitoring
Semantic Search and Intent Keywords
To maximize the reach and relevance of this content, the following semantically related and high-intent keywords should be considered:
| Keyword Type | Keywords |
|---|---|
| Afib/Cardiovascular | atrial fibrillation, irregular heart rhythm, cardiac arrhythmia, stroke risk, heart health monitoring, heart rhythm disorder, cardiovascular health |
| Respiratory/Sleep | sleep apnea symptoms, obstructive sleep apnea (OSA), breathing problems during sleep, low blood oxygen, overnight pulse oximetry, pulmonary health, respiratory failure |
| Wearable Tech/Data | best smartwatches for Afib, fitness tracker heart rate, monitor sleep quality, SpO2 sensor accuracy, continuous heart rate monitoring, smart ring health data |
| Connection/Co-morbidity | Afib and sleep apnea link, connection between heart and lungs, respiratory stress and Afib, comorbidity of heart and lung disease, treating sleep apnea Afib success |
| Intent (Action-Oriented) | what to do if my watch detects Afib, interpret my smartwatch HRV, should I get a sleep study, early detection of heart problems, managing sleep apnea with wearables |
Conclusion: Closing the Cardiopulmonary Loop
The modern wearable tech device is moving past being a simple gadget to becoming a critical element of personalized, preventative medicine. By focusing on Afib detection and tracking metrics like heart rate variability (HRV), these devices offer a window into the holistic health of the cardiopulmonary system. The finding that irregular heart rhythm (Afib) often co-occurs with severe sleep apnea and lung strain is a vital clue, transforming an arrhythmia alert into a potential red flag for broader respiratory stress.
For users, the message is clear: do not dismiss a persistent Afib alert, especially if it occurs at night. Discuss the pattern of your heart data, including HRV and any nocturnal oxygen drops, with your doctor. This data from your wrist is providing invaluable early warning signs and establishing a profound cardiovascular link that allows for effective sleep apnea screening and, ultimately, the prevention of more severe health outcomes. By heeding these subtle signals, your smartwatch may not just be protecting you from stroke; it could be saving your lungs and improving your overall quality of life.